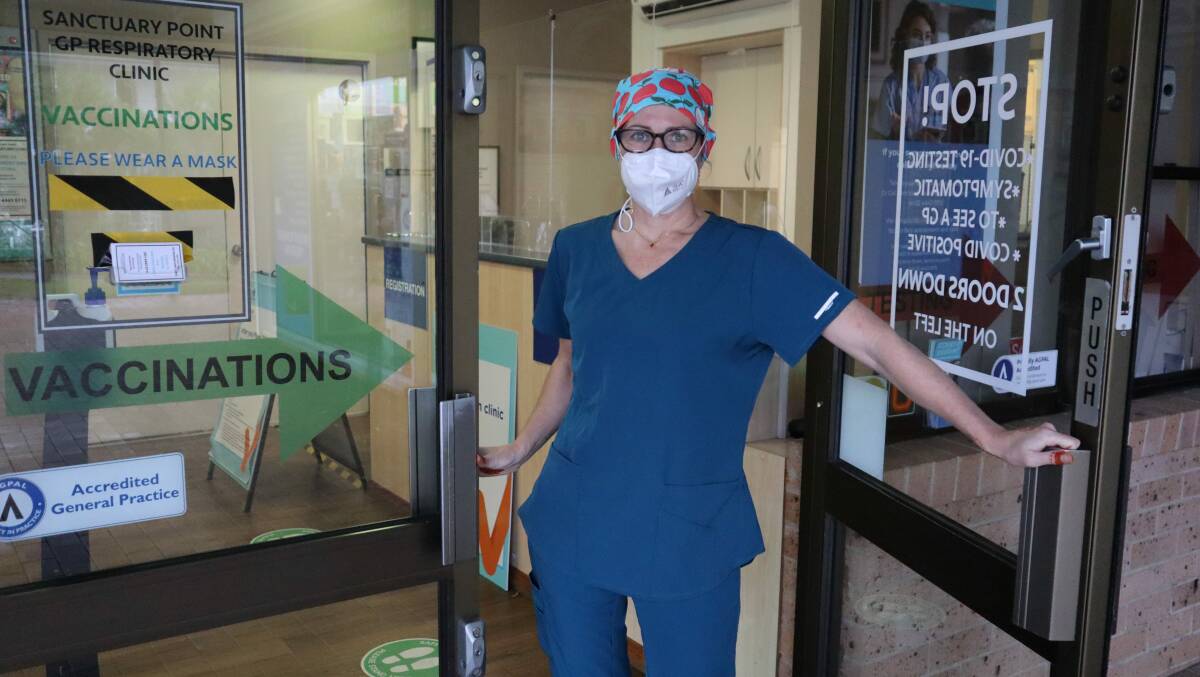
Sanctuary Point Respiratory Clinic has become a rare, yet vital service for patients of the Bay and Basin, and the Shoalhaven at large.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
Since it opened two years ago, more than 30,000 patients have come through the door of this COVID clinic - and they're coming in for more than just testing and vaccinations.
The clinic is also one of the few places locals can go to see a doctor for any ailment, while they are also symptomatic or COVID-positive.
Its importance has been recognised by the local health district, which is sending COVID-positive patients to Sanctuary Point, where possible, to ease the pressure on hospital emergency departments.
Principal GP Dr Kate Manderson said clinic staff don PPE for set sessions during the day, enabling them to treat patients who happen to have COVID.
"The emergency department and local health district now have us as part of their pathway for a COVID-positive person, who is not sick enough to go to hospital but still needs to see someone," she said.
"Of course they can contact their usual GP, but if their GP is not in a position to see them fact-to-fact, they can come in here to us."
Having the dedicated sessions for patients with COVID is aimed at reducing the potential impacts on other local services - in particular, emergency departments.
Dr Manderson noted that the patients they see at the respiratory clinic obviously have COVID concerns, but there are plenty more reasons for them to need a GP.
"We can do everything from listen to their chest and check that they're okay from a COVID perspective, to sometimes they have an ingrown toenail, or a bladder infection, or something completely unrelated," she said
"But of course they can't go in to their normal doctor."
The Sanctuary Point Respiratory Clinic is one of just 150 remaining Commonwealth-funded centres, which opened early in the pandemic.
It has seen, on average, 60 patients a day since it opened two years ago.
Winter is coming, so is the flu
Flu season is coming up fast, and healthcare workers are bracing for a combination of COVID and influenza.
After fairly low numbers of flu cases during previous pandemic years, low immunity to flu viruses is a big concern.
As of Thursday, there were just over 1400 people hospitalised for COVID in New South Wales.
A surge of patients needing hospital treatment for the flu would be yet another strain on resources.
Dr Manderson said it was important to be vaccinated for both COVID and the flu, to reduce the likelihood of hospitalisation.
"Getting vaccinated against both means that when you need emergency surgery, or when your elderly mum falls in the nursing home and needs to have her hip repaired, the hospital will be able to do that and look after her because it won't be chock full of people with COVID and flu."
Clinics still scrambling for doctors
At its peak the Sanctuary Point Respiratory Clinic has run with around 15 staff. On a regular day there will be seven, including four clinicians.
Currently the clinic is open for regular business hours - Monday to Friday, nine to five - but Dr Manderson would like to do more.
She said they face the same roadblock as almost every clinic in Australia: there's simply not enough GPs.
"I don't really have enough staff to cope with demand; we could do more if we had more staff," she said.
"We could open more hours or open on weekends, but that [staffing] is a real challenge for us.
"It's become a bit of an election issues as well, so hopefully that is shining some light on it."
Some systemic changes have removed barriers for bringing in GPs, and Dr Manderson said their own clinic did notice a difference.
However, the health system still faces shortages, and there are concerns for particular areas.
"I can't speak for the other clinics, but the clinics that we do work with and the way we operate has gotten better," she said.
"Instead of being short by five doctors, we're short by three doctors... We're still seeing that ED has more people going in than they should after hours and there's not enough doctors to cover those rosters; the aged care facilities are crying out as well."
Dr Manderson said she would like to see state and federal governments working together to fill "a really big gap" in services for aged care residents who catch COVID.
While the state government is responsible for the health system, aged care falls under the federal government's remit.


